This week the St Emlyn’s team is in Gateshead for the Royal College of Emergency Medicine’s annual scientific conference. This year I’ve been tasked with putting together the top 10 (plus 1) papers of the year.
This is always a bit of a random presentation as what do we mean by ‘Top’? Ask 5 different professors of emergency medicine and you’ll probably get 5 different answers. For me it’s papers that might make a change to clinical practice. Either by changing what we do, or by reinforcing something that we currently do. So the papers below are entirely my choice. You can argue with them and that’s fine. In fact if you think I’ve missed something please suggest your favourite paper in the comments. If the paper you published yourself is not here, then I apologise, I’m sure it was fabulous but I may have just missed it 😉
In truth I did not select these on my own. I asked the St Emlyn’s team and fellow bloggers around the world, notably Chris Hicks, Scott Weingart, Ken Milne, Cliff Reid, Salim Rezzaie and more.
Let’s crack on and in no particular order…..
Paper 1: Do we need to shock AF early?

I’m an enthusiast about cardioverting AF in the ED. For patients coming in with acute onset AF and no reason for not sedating then I’m really keen to get the anaesthetic drugs out in order to deliver a bit electricity to get them back into sinus and on their way. The question is whether we need to do that as urgently as I would like? In this RCT from the US patients were randomised to either early (asap) electrical cardioversion or a delayed approach where they aimed to cardiovert within the 48 hour window.

In the paper the main outcome was whether patients were still in sinus rhythm at 90 days and the result there was that there was no difference. So their argument was it makes no difference.

More interestingly for me was the number of patients who spontaneously cardioverted in the delayed treatment arm of the trial. Roughly two thirds of them spontaneously went back into sinus rhythm. Thus my conclusion is that it’s fine to watch and wait. The argument for asap cardioversion can be made from a in patient bed availability perspective, but that needs to be balanced against the potential risks of sedation and cardioversion.Paper 2
Paper 2: Ventilation during RSI.

For many years I have seen some of my colleagues routinely ventilate patients at risk of desaturation in the time between induction and paralysis taking effect. We typically do this using a Water’s circuit with a bit of PEEP applied (that’s a Mapleson C circuit) which we use for pretty much all RSIs in Virchester). In pre-hospital care there is a preference for the BVM as it still works even if you lose your O2 supply. It’s done gently and carefully to avoid gastric insufflation, but it’s always felt a little odd as we I was originally taught that ventilating at this stage of the RSI was forbidden and dangerous. Notably because it was felt that it could induce aspiration. On the other hand there are the risks of desaturation, hypoxia and the associated consequences of cardiovascular instability and potential end organ damage. Thus the debate about whether ventilating the patient in the time between induction and intubation has been controversial and debated for years.
This paper is an ED based RCT showing that it is safe and advantageous to ventilate patients between induction and laryngoscopy. Far fewer patients desaturated and there was no increase in complications (aspiration and pneumonia). Read more about the paper here.
Paper 3: Cricoid pressure in RSI

This is an RCT in patients undergoing RSI in theatre. Patients were randomised to cricoid or sham cricoid (no pressure) with outcomes of evidence of aspiration at laryngoscopy or on chest Xray. Secondary outcomes were on the difficulty of aspiration.

The bottom line was that there was no difference in terms of airway soiling (0.6% vs. 0.5%), but it was clear that there was evidence of increased difficulty if the patient had cricoid.

Although this is not an EM trial and there were exclusions (e.g. small bowel obstruction) it’s yet more evidence that cricoid may do more harm than good.
Paper 4: Magnesium in AF

This has been a long running debate. Should we give magnesium to patients in fast AF in the ED. This RCT randomised ED patients to adjuvant MgSO4 together with their usual rate/rhythm control drugs. Patients got placebo, 4.5g MgSO4 or 9g MgSO4.

The bottom line is that adjuvant MgSO4 made a real difference, but the higher dose offered no advantages but more side effects. So go with adjuvant MgSO4 for your AF patients.

Paper 5. Levetiracetam vs. Phenytoin for second line treatment in paedaitric epilepsy

This RCT randomised children to children who were still fitting after first line benzos. We reviewed this trial in depth here on the blog, so read that if you want the detailed analysis. Bottom line is that there was little difference, perhaps with a signal that phenytoin was slower to get control.

For us at St Emlyn’s we believe that Levetiracetam is a preferred option as it’s easier to make up and has a better safety profile.

We reviewed this paper on the blog earlier in the year. You can read a full review of the paper (both Eclipse and Concept) here. An RCT of Levetiracetam vs. Phenytoin for children in status epilepticus. The bottom line in the trial was that there was no difference.
Although not a primary aim of the study it’s likely that Phenytoin takes longer to act and in our opinion it’s more tricky to make up and has more side effects. Sadly I’ve been involved in a few drug errors with Phenytoin and so I think there are pragmatic reasons why we might want to move to Levetiracetam.
Paper 6: Does POCUS make a difference in Cardiac Arrest?

I’m a big fan of ultrasound in the emergency department and have been on record as saying it’s an essential skill for the resus room (it was a bit controversial and lost me some friends), but in truth the evidence to underpin my assertions has been fairly scant. In cardiac arrest patients I use it to look for treatable causes and in those patients with electrical activity I use it to assess whether there is any associated mechanical contraction. But does it make a difference?
The SHOCK ED3 trial aimed to answer this. There are lots of biases in this observational single centre trial but it is evidence of how POCUS might change resus room management.

Yes it’s retrospective, yes it’s single centre and retrospective but the results are interesting. POCUS frequently changes management as evidenced by additional procedures AND it is associated with increased rates of ROSC.


Sadly the increased rates of intervention were not associated with increased survival and if you are a USS skeptic I’m sure that you’ll find that the most important outcome (Ed – because it is), but for me it is evidence of the need for USS skills by EM docs.
Paper 7. Are vasopressors contraindicated in haemorrhagic shock?

The answer, if you are in the UK at least, is yes. This is something that we don’t do in the early phases of haemorrhagic shock. However, when we did a simulation competition at the EuSEM conference in Glasgow we were surprised to find that many of our European colleagues do use vasoconstrictive inotropes far earlier than we do. This year there is an interesting paper in JAMA, an RCT in fact, looking at the early use of Vasopressin in trauma patients.

Interestingly the trial found improved outcomes in those treated with Vasopressin. However, the outcomes were around the use of blood products rather than more patient orientated outcomes like death (which was 12% in both groups).
Paper 8: Early vasopressors in septic shock

The Censor trial comes on the back of a general move towards earlier use of vasopressors in septic shock. This is something that many sepsis afficionados have been pushing for several years. In Virchester we start considering vasopressors after 2L of IV fluids, or at least we think we do. Whilst we imagine that the days of 6-10L of IV fluids for the septic shock patient in the first few hours are gone, we are not naive enough to think that it never happens, especially in those patients who are not heading straight to ICU.

In this RCT, 310 patients were randomised to early noradrenaline vs. placebo. Although this was single centre and in Cambodia, factors which limit the applicability of the findings, they are interesting.

Patients with early noradrenaline had less shock and less pulmonary oedema than those receiving placebo. Sadly the trial was not big enough to definitively find a mortality benefit, but it was better in the noradrenaline group.
Paper 9: Does every cardiac arrest patient need to go to the cath lab?

In the ED we often focus out learning and skills on improving our ability to get ROSC, but what next? If we get ROSC should the patient go to ICU, CCU or direct to the cath lab? This is a real question as moving patients to the cath lab is not always straightforward as they be quite unstable and in some centres it may be tricky to manage things like temperature control.
For those patients who have ST elevation on the post ROSC ECG I don’t think there is any argument – they go straight to the cath lab. What about those without ST elevation though?

The COACT trial looked specifically at this. An RCT of 552 patients randomised to either immediate cath lab transfer or a more delayed approach.
So the bottom line appears that there is no real need to go direct to cath lab in this group. Probably because they represent a broad range of pathologies and that’s important because this does not mean that in practice none of these patients should be directly transferred. It does mean that you should stop and think. For example, the patient with prior ischaemic symptoms is different from the 24 year old athlete who collapsed whilst playing football. The first should go, the second maybe not just yet.
Paper 10: Diagnosing PE in pregnancy

The pregnant patient with a potential PE is a diagnostic conundrum. We know that tests such as d-dimers are not as helpful in this group and yet the patients are at higher risk and the consequences potentially awful. I’ve seen a variety of approaches to this over the years, but at the moment it usually involves bloods, a chest x-ray, ultrasound for DVTs and then a chat. V/Q is then the way to go with CTPA reserved for a small number of cases.

In some health economies I think CTPA is more common in this group and is may be rising as access to CTPA becomes easier, even though few people think more CTPAs in this group is a good idea!
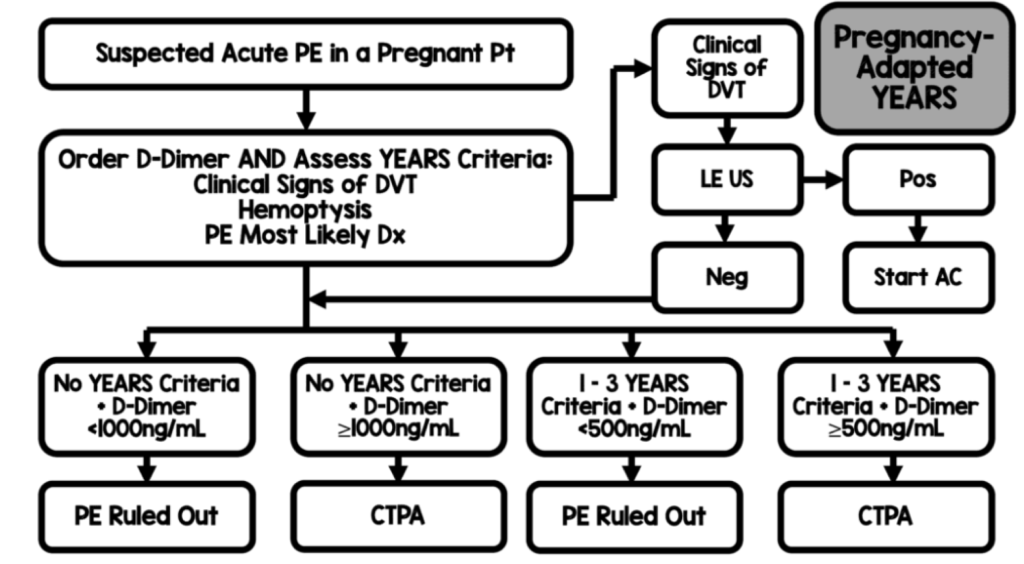
The YEARS study looked to exclude PE in patients who had no signs of DVT, no haemoptysis and in whom the clinician felt that PE was an unlikely diagnosis. This study adapted the YEARS algorithm for use in pregnant women and then followed 496 patients through to determine the utility of the approach.

Overall the sensitivity was good, although there were small numbers of positive patients in the trial. In terms of CTPA use this study showed a reduction, but be cautious on this. It’s only a reduction if you did lots before. In my practice I would worry that this may increase usage.
Paper 10: The Zero Point Survey
Cheekily I added the zero point survey paper that I co-authored in 201831–33. Why you may ask? It’s because of all the things I’ve done this year it’s the easiest, quickest, cheapest and most effective to deliver in practice.

We don’t have the evidence yet, but it makes sense and I’d strongly recommend you consider putting it into your practice. Read more about the ZPS here.
Thanks for getting this far. For those in the audience I hope you enjoyed the talk and the emojis.
vb
S
- Early or Delayed Cardioversion in Recent-Onset Atrial Fibrillation https://www.nejm.org/doi/full/10.1056/NEJMoa1900353
- Effect of Cricoid Pressure Compared With a Sham Procedure in the Rapid Sequence Induction of AnesthesiaThe IRIS Randomized Clinical Trial https://jamanetwork.com/journals/jamasurgery/fullarticle/2708019
- Bag mask ventilation during tracheal intubation of critically ill patients. https://www.nejm.org/doi/full/10.1056/NEJMoa1812405#targetText=These%20results%20suggest%20that%20for,severe%20hypoxemia%20in%20one%20patient.&targetText=It%20has%20been%20hypothesized%20that,of%20aspiration%20during%20tracheal%20intubation.
- Low-dose Magnesium Sulfate Versus High Dose in the Early Management of Rapid Atrial Fibrillation: Randomized Controlled Double-blind Study (LOMAGHI Study). https://www.ncbi.nlm.nih.gov/pubmed/30025177
- Levetiracetam versus phenytoin for second-line treatment of paediatric convulsive status epilepticus (EcLiPSE): a multicentre, open-label, randomised trial. https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(19)30724-X/fulltext
- Does Point-of-care Ultrasound Use Impact Resuscitation Length, Rates of Intervention, and Clinical Outcomes During Cardiac Arrest? https://www.cureus.com/articles/18740-does-point-of-care-ultrasound-use-impact-resuscitation-length-rates-of-intervention-and-clinical-outcomes-during-cardiac-arrest-a-study-from-the-sonography-in-hypotension-and-cardiac-arrest-in-the-emergency-department-shoc-ed-investigators
- Effect of Low-Dose Supplementation of Arginine Vasopressin on Need for Blood Product Transfusions in Patients with Trauma and Hemorrhagic Shock: A Randomized Clinical Trial (AVERT Shock). https://www.thebottomline.org.uk/summaries/avert-shock/
- Early Use of Norepinephrine in Septic Shock Resuscitation (CENSER). A Randomized Trial. https://www.ncbi.nlm.nih.gov/pubmed/30704260
- Lemkes JS, Janssens GN, van der Hoeven NW, et al. Coronary Angiography after Cardiac Arrest without ST-Segment Elevation. N Engl J Med. March 2019. doi:10.1056/nejmoa1816897
- Pregnancy-Adapted YEARS Algorithm for Diagnosis of Suspected Pulmonary Embolism https://www.nejm.org/doi/full/10.1056/NEJMoa1813865
- Zero Point Survey.


Pingback: #RCEMasc 2019 – Day 2 – EMbeds.co.uk
Pingback: #RCEMasc 2019 Day 2 • St Emlyn's
Thanks Simon
Paper 4 and 10 sounds very interesting
BW
Maad
A trainee has just pointed out that Paper 1 follow up was up to 30 days (not 90). I think the message stands, however. Great selection of papers.
Pingback: October 2019 Podcast round up. St Emlyn's • St Emlyn's
Pingback: JC: Critical care reviews meeting day 1 #CCR20. St Emlyn's • St Emlyn's